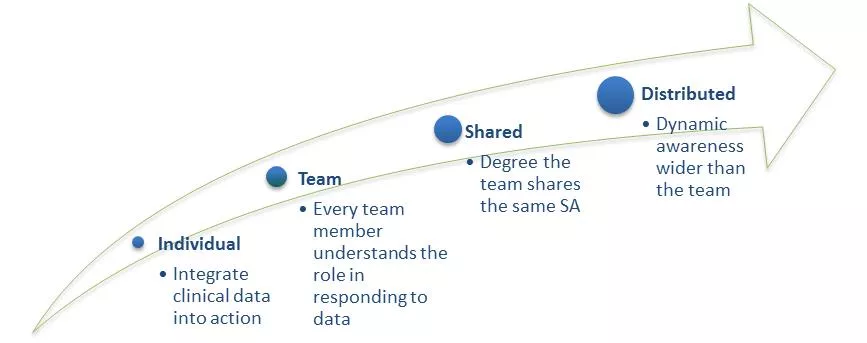
A key component of introducing situation awareness is having reliable mechanisms for communicating within the team. This section also provides an outline of the importance of structured communication and some tools that can help embed it.
Identifying deterioration early
It is often difficult to detect deterioration early, particularly in sepsis. Therefore, we need to change the way we look at children to see if we can increase our awareness of potential deterioration.
Five risk factors are associated with preventing deterioration, as detailed in studies from Cincinnati Children's Hospital and Medical Centre1.
- Family concerns should always be taken seriously, even if vital signs are normal.
- High-risk therapies raise the risk and make the child a potential candidate for deterioration.
- Presence of an elevated early warning score is a marker, though it is not always present.
- Watcher/clinician gut feeling is where any member of staff senses that the child is not right.
- Concerns about communication with the patient, parent or their family are discussed (eg they speak a different language to you and your team).
You can download the presentation - closing the gap in paediatric safety below. This gives a brief overview of some of the main components used in recognising and responding to deterioration and can be used as an introduction. However, most information is included with the suggested tools that follow.
Identifying deterioration early - tools
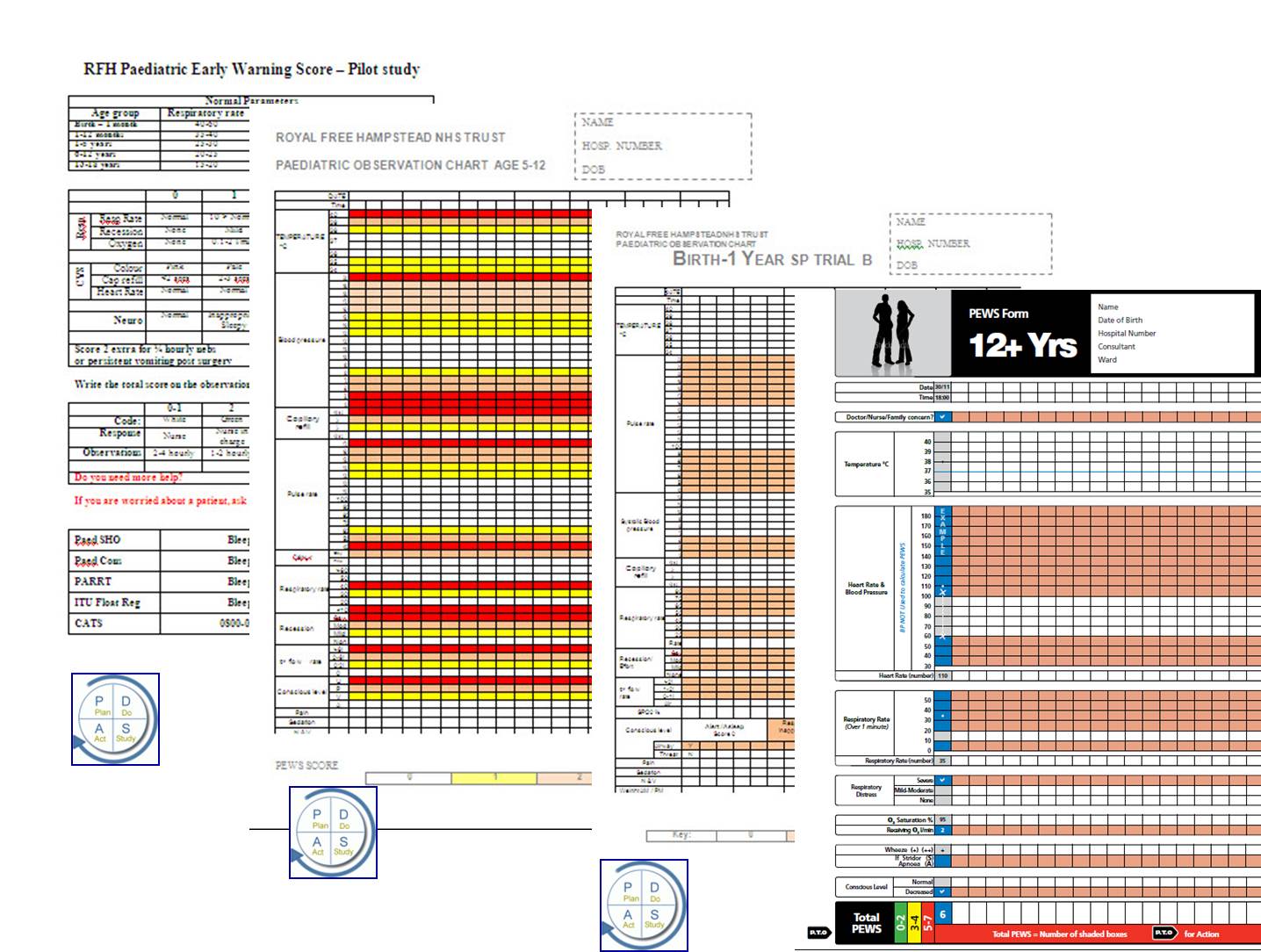
Paediatric Early Warning Score (PEWS) and systems
The main tool for recognising and responding to deterioration in children is a Paediatric Early Warning Score or System (PEWS). There is a variety in use across the country, but two examples have been selected below. In addition, there is a list of the PEWS each S.A.F.E site is using. There are also tools for reviewing cases of unrecognised deterioration and specific causes of deterioration which will help you provide learning to your team.
There is no perfect PEWS. The key is to have good observations and to use one consistently, bearing in mind the tool is designed to be sensitive but may lack specificity.
The score is part of a system incorporating all of the above. If one recognises the limitations of the PEWS then its value increases as part of a system. Nurses need to be trained in standardised observations and doctors in responding to the PEWS.
The NHS Insititute for Innovation and Improvement (NHS III) described PEWS as follows:
Early warning scores are generated by combining the scores from a selection of routine observations of patients e.g. pulse, respiratory rate, respiratory distress, conscious level. Different observations are selected for children and adults due to their naturally different physiological responses. If a child's clinical condition is deteriorating the 'score' for the observations will (usually) increase and so a higher or increasing score gives an early indication that intervention may be required. Early intervention can 'fix' problems and can avoid the need to transfer a child to a higher level of care and thus avoid or reduce harm.
You can access the PIPSQC work on PEWS to download charts, videos and guidance. This is only one example; other PEWS, and variations on these PEWS, are available. For example Evelina London Children's Hospital use a threshold/trigger based system.
You can download an example PEWS poster below.
RECALL tool
The RECALL (Rapid Evaluation of Cardio-respiratory Arrests with Lessons for Learning) tool was developed at Great Ormond Street Hospital to allow real-time analysis of deterioration by asking a number of key questions after a child deteriorates. This allows the clinical team to mitigate and change processes to prevent the next deterioration2.
Part 1 allows for the evaluation of deterioration. This considers the assessment of the patient in the previous 24 hours and the escalation in response to the deterioration, clinical reviews and interventions, with any lessons for learning identified.
You can download RECALL forms from Great Ormond Street Hospital below. Note that Part 2 form provides an opportunity for the clinical lead to review the deterioration and gather any additional information. Based on this, a decision is made to either accept the report with changes, or to gather further information.
You can download two example posters from S.A.F.E sites that used RECALL below.
Re-ACT
NHS England has prepared resources, including a number of short videos, that address key areas which need to be considered in developing a programme to decrease unexpected deterioration.
It covers the following broad themes: parent/carer engagement; health care professional education; systems improvement; score and system design; reducing term admissions to neonatal units.
See Re-ACT (Responding to Ailing Children Tool)
Using structured communication
To achieve non-hierarchichal communication within a microsystem, it is useful to agree on a structured approach to communication.
The main benefit is to help embed a reliable transfer of information, providing a framework for the information that needs to be communicated. This approach can also be used to allow individuals who may not fully understand what has been said to pause the conversation and have the information repeated.
The underlying principle is to introduce and embed a structured way for staff to provide accurate information and to be able to challenge potentially unsafe processes in a protected and constructive way.
Some examples of structured communication
- Can I have clarity?: This indicates that the process or communication is not clear and provides a pause. This allows the process to be rechecked and reviewed, or the conversation to be repeated, before being restarted once everything is clear.
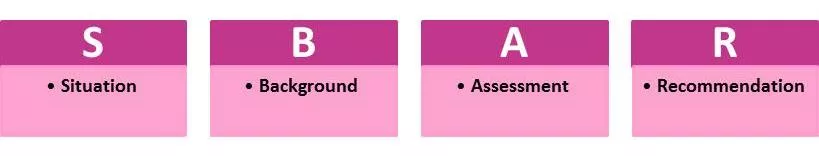
- SBAR (Situation Background Assessment Recommendation): As shown in the diagram below, this provides a non-threatening and easy-to-follow framework to improve communication and lead to a decision.
- ISBAR is a variation, where I stands for Identify. Introducing ISBAR is like learning a new language and as such, will require practice, role-play and an adherence to a new way of communicating.
You can download our Presentation - using structured communication below.
Using structured communication - tools
Implementing structured communication can be difficult, especially to get to a position where it is used reliably and consistently.
S.A.F.E recommends two key tools, SBAR and CUSS, but we recognise that there are many variations on the same themes. The main message is to understand structured communications and find a tool that suits you.
Situation, Background, Assessment, Recommendation (SBAR)
The NHS Institute for Innovation and Improvement (NHS III) described SBAR as a structured method for communicating critical information that requires immediate attention and action, contributing to effective escalation and increased patient safety. Used with PEWS (covered in the next section), it can help staff to escalate a concern when the PEWS indicates the need for additional intervention.
The way in which SBAR is introduced will determine the extent to which it is adopted. SBAR can be used effectively to enhance handovers between shifts, or between staff in the same or different clinical areas.
SBAR is an area where you may see some variation. You may find it prefaced with an I (Identify) to prompt an active introduction at the start of the handover. Or, a D (Decision) to ensure any decision taken is repeated and noted down. You may see both.
Concern, Uncomfortable, unSafe, Stop (CUSS)
Similar in some ways to the "Can I have clarity" question, in that it allows someone to express concern regarding an instruction or process in a non-threatening way, CUSS provides a levelled and assertive approach to raising concern.
- You can download our Presentation - the CUSS communication tool below.
The huddle
The huddle is the core intervention. It aims to change the way you approach the care of children from reaction to anticipation. It is proactive and allows the sharing of information.
The underlying premise is that everyone around the child from parent, administrative and support staff, students, nurses doctors and allied professionals have a different lens or view on how the child is doing and everyone’s voice needs to be heard. It is structured and lasts a short time. Therefore, there are scripts appropriate for the clinical area. All need to be trained in the methodology to ensure it does not become a ward round.
What does implementing the huddle allow?
- Proactive identification of risk ahead of deterioration
- Unit-based huddles on a regular basis, starting at the bedside with the nurse, doctor and patient
- Three to four inpatient ward huddles each day to provide collective understanding and shared insight
- Unit or divisional huddles as well as a hospital-wide huddle
- Continuous learning system to evaluate situation awareness at all levels
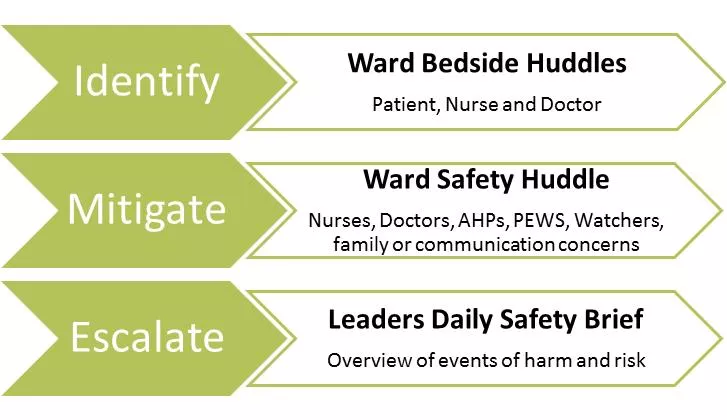
Types of huddle
Much of S.A.F.E has focused on the Ward Safety Huddle. However, in recent months, teams have expanded to include both the Ward Bedside Huddles and the Leaders Daily Safety Brief.
Scripts
Sets of questions that can be added are aimed at ascertaining the safety at any given time. The daily questions to be asked at different levels - ward, unit, division and hospital - are:
- What did we do well? So that we can replicate this elsewhere.
- Is there any past harm? Has patient care been safe in the past 4, 6, 12 and 24 hours?
- How reliable are we? Are our clinical systems and processes reliable?
- Are we sensitive to today's operations? Is the care we are delivering today safe?
- Are we anticipating and preparing? Will the care we deliver be safe in the future?
- Are we reviewing and learning from current and past operations? Are we responding and improving?
You can download our Ward Safety Huddle scripts below. You can modify these so they are more suitable for other Huddles.
Responsibilities
The huddle - tools
As discussed, the huddle is a key intervention for introducing situation awareness, especially as part of a structured approach to communication in a given day. The tools and resources below will help you embed situation awareness as part of your local project.
Huddle scripts and trigger tools
To implement your huddles, there are two tools that you will find useful.
- Script - This outlines the process that will be followed during each huddle. This tends to be a list of questions used to prompt patients to be discussed. Here are three examples, but we encourage you to develop your own.
- Trigger tool - Essentially, this builds a second step into the huddle process, but allows someone, usually the Nurse in Charge, to go around the ward before the huddle and identify which patients will trigger a discussion at the huddle. This means that when at the huddle, only triggered patients are discussed.
You can download three example scripts and one trigger tool below.
Drug-gle
This huddle is developed to discuss medications. The medical and nursing staff meet with the pharmacist regularly to review medication harm, risks and near misses, so that processes can be improved.
The Drug-gle has been one of the major successes of S.A.F.E, with it spreading across multiple participating sites.
You can download two example Drug-gle posters below.
Huddle Reflection Tool
Developed by the S.A.F.E Evaluation Team, the Huddle Reflection Tool helps you assess the quality of a huddle.
Focusing in on four specific areas (structure, environment, collaborative culture and risk management), it is designed to give a point-in-time evaluation of the huddle and helps identify potential areas for improvement.
In early days, you might wish to use the tool frequently, perhaps daily as part of your PDSA cycles. However, as huddles become more embedded, the tool can be used less frequently, as a means of auditing the quality of your huddles.
You can download the huddle reflect tool below.
Parent and CYP engagement
Parents, and children and young people themselves, are an important resource, and a number of interventions have been developed for them. Examples of tools that have been developed by S.A.F.E sites include:
- Daily goals: Identifying specific goals for each patient for a given day
- Whiteboards: Providing whiteboards to help communication with patients, parents and families
- Information posters: To provide parents and families with information about S.A.F.E
You can download examples of materials developed for patients, parents and families, to raise awareness of S.A.F.E and encourage their involvement, below.
- 1Brady et al,. Improving Situation Awareness to Reduce Unrecognized Clinical Deterioration and Serious Safety Events. Pediatrics, 2013. 131; e298-e308
- 2Runnacles et al., RECALL (Rapid Evaluation of Cardio-Respiratory Arrests with Lessons For Learning): Developing a Tool to Learn from Paediatric Arrests. Arch Dis Child 2013;98:A56 doi:10.1136/archdischild-2013-304107.131