Theories of patient safety
Patient safety is a fundamental part of quality care. The aim is to provide reliable care and constantly learn from the daily care being provided.
The basis of the process is the development of high reliability processes in the clinical microsystem. This involves anticipation of what may happen and resilience when things do occur, which forms the basis of situation awareness.
We build our approach to patient safety on four key steps1, 2:
- Risk management - to identify risks and adverse events and to develop a response to mitigate that risk.
- Human factors - addressing the factors that can cause harm due to the nature of humans. This includes addressing the design of processes to take these risks into account, looking at tasks, equipment, environment, patients, and staff factors and how they impact on safety.
- Reliability theory - aims to develop standardised approaches and have the patient receive the right care the first time every time.
- Resilience engineering - looks at what works and tries to build on this as well as learning from what doesn't work.
Model of accident causation
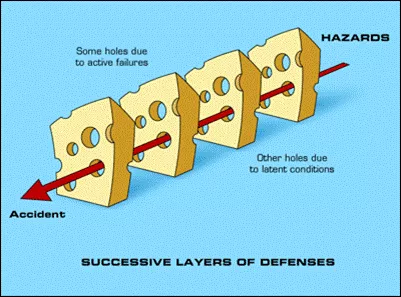
In focusing on patient safety, we put in place a number of barriers that are designed to prevent harm from reaching the patient. However, each of these barriers has weaknesses, and occasionally the barrier is breached. Patients are harmed when successive barriers to harm are breached.
One way of looking at it is described by Reason's Swiss Cheese Model of Accident Causation, shown below.
Presentation and papers
You can download the presentation on patient safety culture below. This gives an overview of the theories of patient safety, including how to develop your own safety-based culture.
You can also find more information in a series of free online papers and theories of patient safety on Springer Link.
And, you can look at a paper from the Health Foundation, which provides a framework for patient safety.
Tools
Understanding the theories that underpin the concept of patient safety will be key to helping identify the specific aim of your local project. It will also give you a deeper understanding of how to measure and improve the local safety culture.
The tools below, including some worked examples, have been selected to help you understand the local culture, and identify areas for further improvement.
Manchester Patient Safety Framework (MaPSaF)
This online safety tool helps you assess how a team views the approach to safety. It can also be used as a developmental tool for team building, as well as help begin a journey to open communication.
Safety climate survey
Modified for UK healthcare from the SCORE Survey, this aims to provide an indication of the safety culture on a ward. The staff survey is is usually administered every six months. It allows you to measure changes in the cultural attitudes.
You can download the safety climate survey and guidance below. You can also read a report about the SCORE survey and an overview of patient safety measurement.
Experience of care survey
A key component of S.A.F.E is engaging with children and young people and their parents and families. It is equally important to involve them with understanding the safety climate as it is in the specifics of their particular reason for being in hospital.
You can download our experience of care survey for young people 9 to 18 years and for parents below.
SHINE tool
This tool, developed at Great Ormond Street Hospital, allows parents to report potential harm in real time. It adds a new dimension to understanding harm on the ward.
You can read full details in an article, with information on accessing the tool (PDF).