Emergency departments across the UK are seeing very high numbers of young children for this time of the year because of a rise in infections usually seen in the winter. One emergency paediatrician described the situation as “winter in June”. Three Royal Colleges are issuing advice for parents concerned about fever in their child.
The Royal College of Paediatrics and Child Health (RCPCH) has heard from paediatric emergency medicine doctors around the country describing pressures on their emergency department (ED) from an increase in children being brought in with mild fever by anxious parents. Many parents have not seen fever in their child – particularly if they were born during lockdown – and are taking them to A&E rather than seeking help at pharmacies, their GP, NHS 111 or online.
Describing the rise, Dr Dan Magnus, consultant in Paediatric Emergency Medicine at the Bristol Royal Hospital for Children commented:
We had an incredibly busy week last week – in fact on Monday we set a new record for the number of children seen in 24hrs in our department ever, and that’s in the middle of summer. We are effectively running a winter-level ED response in the summertime.
Dr Richard Burridge, consultant paediatrician, lead for the children’s emergency department, Watford General, said:
We’re seeing three times the number of children with fevers for early June than in 2020 – which was lower because of COVID – and twice the number of children we saw in June 2019, significantly higher than we’ve ever seen before in children’s ED.
The increase in cases of children with fever is related to a rise in respiratory infections such as RSV (respiratory synctial virus) and bronchiolitis, paraflu, and rhinovirus, all of which produce symptoms of coughs, runny nose and fever. These infections, which are usually mild, are mostly seen in the winter months, but the easing of lockdown has meant that children are being exposed to them this summer as they come back into contact with other children.
The RCPCH, the Royal College of Emergency Medicine (RCEM) and the Royal College of GPs (RCGPs), have issued advice on how parents can treat children with mild fever and when to seek help.
Dr Camilla Kingdon, President of the RCPCH, said:
Many emergency departments are currently overwhelmed and there has been a particularly steep rise in the number of young children presenting. Some have seen the highest ever numbers of children in their department and waiting times can be huge.
The biggest increase we’re seeing is in children with mild fever. Fevers are very common in young children and usually aren’t serious. But many parents haven’t seen fever in their child before and are worried, particularly if they don’t have their usual sources of support to turn to, such as parent groups.
Most of these children are fine and have returned home once their parents were reassured. But that takes time. With departments already under huge pressure, we need to make sure that services are available for children who are seriously unwell.
Dr Michelle Jacobs, from the RCEM Paediatric Emergency Medicine Professional Advisory Group, said:
Emergency departments (EDs) are currently under intense pressures, with many sites reporting record breaking numbers of patients, crowded departments, and long delays, putting patient safety at risk.
We know there has been a sharp increase in children under-5 presenting. The majority of these young children are mostly well, but with a mild fever.
We absolutely understand and recognize that parents may be concerned, especially if their child is young and this is the first time that they have been unwell. But if they take their child to the Emergency Department there may be a long delay, potentially over four hours, before being seen which may be difficult and distressing for both parents and children.
Professor Martin Marshall, Chair of the Royal College of GPs, said:
In an emergency, as outlined in this advice from our three Colleges, A&E is the appropriate place to take a child. We hope this guidance will help parents to be able to make a decision about what is an emergency. In most cases of mild fever, runny nose or cough, simple self-care measures such as taking paracetamol or ibuprofen can help, but in cases where parents are concerned, seeking medical assistance from a pharmacist, their GP or by calling 111 is the appropriate first port of call.
GPs and our teams are under huge pressure at the moment but delivering care to young children is an essential part of our job, and we see tens of thousands of children in general practice every day. We understand that it's a really difficult time to be a parent of a young child, particularly if the child has been born during the pandemic, as many of the usual support services parents rely on have not been available, and we hope they find this guidance helpful when making decisions about their child’s health.
Advice for parents and carers on fever in children
For most children, treatment with children’s paracetamol (eg Calpol®) or ibuprofen (but not both at the same time) is usually enough to reduce the fever and the child will start to feel better after a few days. Ensure your child stays hydrated by drinking clear fluids like water or squash.
Parents who are concerned about fever in their child should call their GP practice or, outside of normal hours, call 111 or the GP out of hours service. Pharmacies can also advise parents.
Always seek medical advice or bring the child in to A&E if:
- Your baby is under 3 months old and has a temperature of 38°C (101°F) or higher
- Your baby is 3 to 6 months old and has a temperature of 39°C (102°F) or higher
- You think your child is not drinking well or is dehydrated. For a baby, this means that they are taking less than half of their normal feeds and having less than two wet nappies a day
- Your child develops a red rash that doesn't fade when a glass is rolled over it
- Your child has a fit (convulsion)
- Your child is crying constantly and you can't console or distract them, or the cry doesn't sound like their normal cry (such as high pitched)
- The fever lasts for more than 5 days or the child is becoming more unwell
Attendances
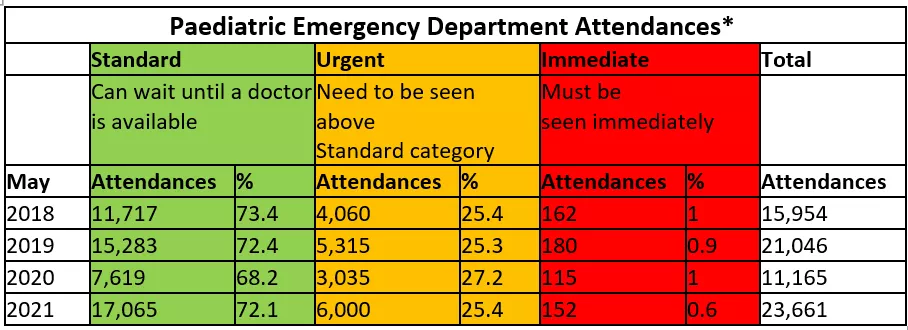
*Composite data of attendances in age group 0-15 years at: Leicester Royal Infirmary, Royal Hospital for Children Glasgow, Birmingham Children's Hospital, and Alder Hey Children's NHS Foundation Trust. Data compiled by Dr Damian Roland, National SPOT (system-wide paediatric observation tracking) Programme.
To speak to ED doctors from around the UK about what they are seeing, please contact the press office: press.office@rcpch.ac.uk.








