What was the challenge?
The challenges we faced over the winter period included having only one registrar to cover both the paediatrics department and NICU (Neonatal Intensive Care Unit) overnight, increasing attendance rate to the Children’s Emergency Department (CED) and poor patient flow throughout the department.
This led to patient safety concerns as well as poor staff morale.
What did you do?
We analysed CED data and breach activity, crash call data overnight and trainee feedback to structure a business case for a range of ‘winter pressure initiatives’. We proposed a series of measures:
- Winter Pressure Registrar to work solely in CAU (Children's Assessment Unit) for eight hours overnight (October – March): Funding was secured by demonstrating the long wait times in CED and the associated high breach rate, and the cost-benefit of preventing such breaches. Funding came from the annual winter pressure budget afforded to the Trust (of approximately £120,000 per year). The cost of locum registrars for six months was projected to cost £75-80,000.
- Paediatric Decision Unit (PDU): This was an additional three cubicle spaces in the CED and CAU. Converting consultation cubicles from ‘paediatric minor injuries’ into PDU cubicles. No cost involved.
- Increasing band 5 and 6 nursing staff (for PDU and CAU): Recruitment drive through social media and through visits to local universities. We supported and mentored nursing students in their placements and aimed to inspire them to return to the department. We employed 2.5 band-5 nurses using money from the winter pressure budget.
- Improved ward clerk support: Helping to streamline the admission and discharge process.
Winter Pressure Registrars
- Eight-hour locum shifts available every night over a six-month period (October – March). The start time was flexible; either 10pm, 11pm or midnight.
- A consultant and middle grade trainee were assigned to managing the winter pressure rota allowing a direct clinical point of contact for locums. We utilised our network of past trainees and connected via social media platforms and messaging applications to advertise and book shifts.
- There was a 96% fill rate of shifts.
- Feedback from the locums included that they liked the flexibility of hours and the ease of communication when booking shifts. Overwhelmingly they felt being the second registrar overnight made the department feel safer and hence they were much more likely to book shifts again.
Paediatric Decision Unit
- Low risk patients awaiting results and requiring a period of observation (where this is predicted to exceed more than four hours and hence would otherwise result in an ‘admission’ or ‘breach’) are observed in PDU.
- Children can be observed for 8 hours before a final decision has to be made.
- Supports the flow of patients through CED.
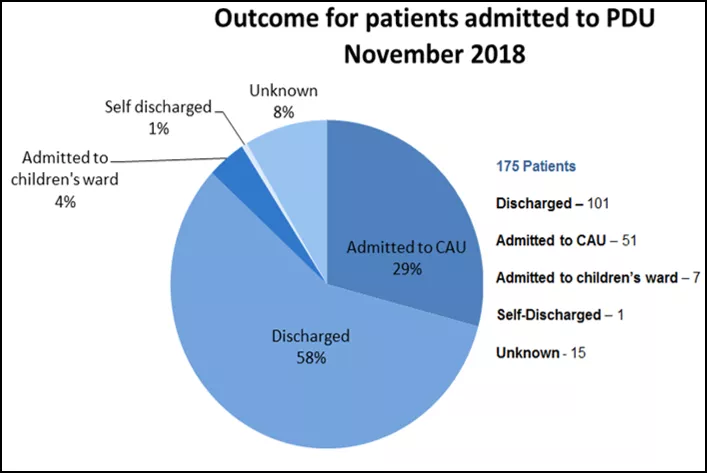
- The outcome of these patients (from November 2019) are demonstrated in Figure 1, below.
- Only one third of children observed in PDU were subsequently admitted to CAU/paediatrics. Without PDU it is likely that 100% of these patients (N= 175 for November 2018) would have had to either be ‘admitted’ or would have ‘breached’.
- Nearly 60% (N=101) of patients were discharged home from PDU in November 2018.
- It reduced the work load on the paediatrics team, reduced the pressure on the CED team and helped to streamline the discharge process.
What impact did these initiatives have?
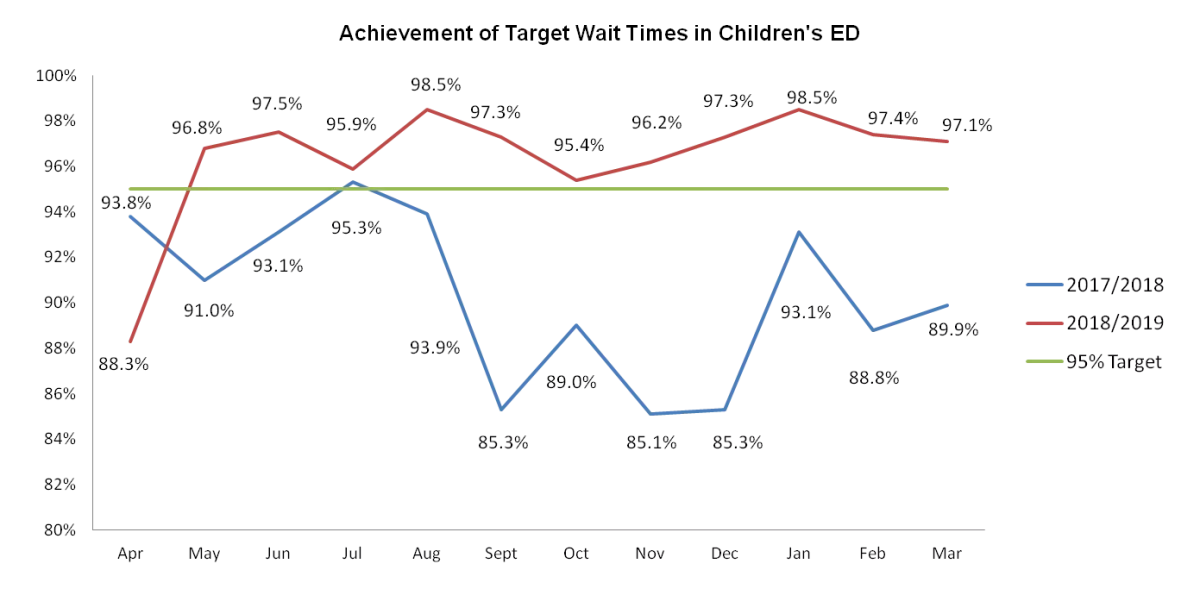
- Breach targets for CED were met every month over the winter period (see Figure 2).
- Nursing vacancy decreased from 35% to 10%.
- 96% locum fill rate for the winter pressure registrar. 174 shifts were booked over 6 months.
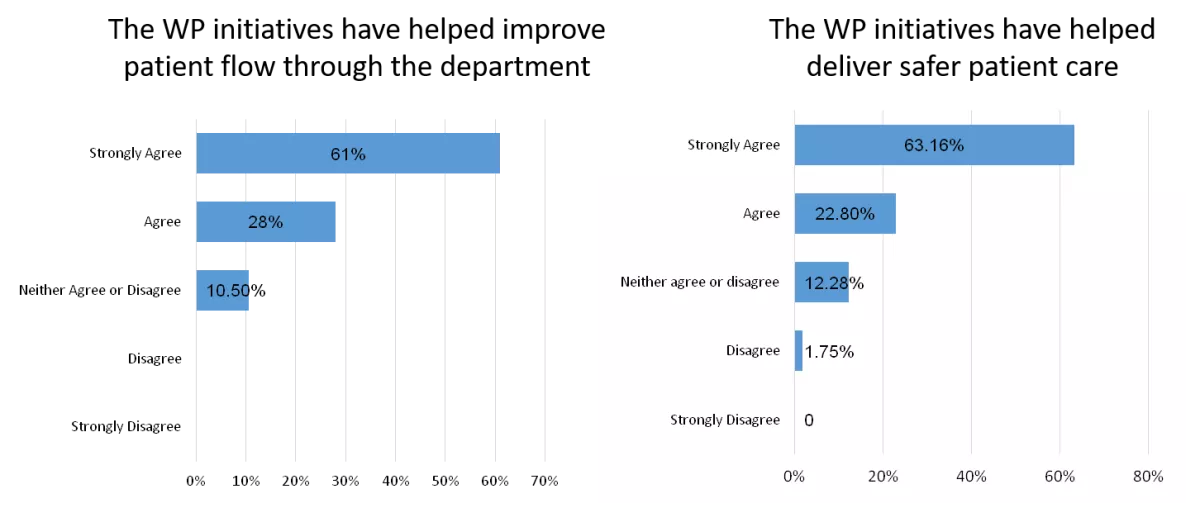
- Significant impact on staff morale. Both nurses and doctors were surveyed about the winter pressure initiatives (see Figures 3 and 4). 89% felt this had helped improve patient flow through the department. 86% felt that safer patient care was delivered as a result of the initiatives and 79% felt staff morale had improved.
What were the challenges in setting this up?
- Gaining funding for extra nurses and six months of locum doctors every night required a very strong business case. It took time to analyse a significant amount of data to formulate this and involved meeting with divisional and nursing leads on a number of occasions.
- Organising the locum rota and advertising and booking shifts took a lot of personal time and dedication from the clinicians (consultant and registrar) involved.
- Locum access, computer logins and orientation for locum registrars coming out-of-hours and during busy times.
What advice can you share?
- Good data collection helps to build a strong business case. Take time to analyse admission and breach data.
- Engage with managers and departmental leads in both paediatrics and emergency care.
- Embrace social media and messaging applications to build links with ex-trainees and locums – it is possible to book a locum every night for six months!
- Inspire and build links with nursing students so they want to come back and work within your team – this is vital to help overcome the recruitment issues often experienced in hospitals.
- Ensure there is a clinical link and personal touch when booking locum doctors – make them feel welcome and valued.
- Team working, planning and strong leadership were the key to our success!
For further information please email amitabhgite@nhs.net
Disclaimer: RCPCH have been notified that the above is a good example in managing winter pressures in emergency departments and will be reviewed on a regular basis. Sharing examples does not equate to formal RCPCH endorsement.