Introduction
This is the first formal release of Round 3 clinical audit data for cohort 1 and the second publication of paediatric epilepsy services organisational data of the Epilepsy12 audit. This is a combined report of the organisational and clinical audits.
The results are of the organisation of paediatric epilepsy services for children and young people in England and Wales as described at November 2019, and the standard of clinical care provided by services that focuses on patients with a new diagnosis of epilepsy between 12 July 2018 – 30 November 2018 for cohort 1.
Within the clinical audit, there are 12 measures which were derived from national guidelines and recommendations. These are referred to as the ‘Performance Indicators’ in the full results presented in Appendices A and G. (Download the Appendices A&G that contain the reports' full results.)
Read our key messages and download our summary report plus detailed audit results below.
Executive summary
Epilepsy is the most common significant long-term neurological condition of childhood and affects an estimated 112,000 children and young people in the UK.1 The State of Child Health2 has highlighted some key trends in paediatric epilepsy, showing that prevalence of epilepsy has reduced in recent years which may partly reflect more specific diagnosis and that there has been progress towards closing the inequality gap in emergency admissions for children with epilepsy. Epilepsy12 (the National Clinical Audit of Seizures and Epilepsies for Children and Young People) uses data collected from hospitals and clinics to support further quality improvement in paediatric epilepsy services.
Epilepsy12 supports the work of the Organisation of Paediatric Epilepsy Networks in the UK (OPEN UK), established in 2015 to join up Health Boards and Trusts into functioning regional paediatric epilepsy networks to encourage and stimulate quality improvement.
The RCPCH Epilepsy Quality Improvement Programme (EQIP) launched on 17 June 2019 and has been designed as a model for a comprehensive Quality Improvement (QI) programme, tailored to support paediatric epilepsy teams to work together to define their shared aims and identify current gaps in service provision. See chapter 5 of the summary report for more information on the programme. And visit the EQIP web page for updated information on the teams’ journeys.
The Epilepsy12 Youth Advocates have been developing a new quality improvement project relating to “Clinic Checks”. A pilot has been taking place in paediatric epilepsy services across England and Wales to assess the support that they provide to young people for their anxieties and worries. See chapter 4 of the summary report for more information on the Youth Advocates.
Key messages
There are some very positive results. Children and young people with epilepsy are receiving care from specialist paediatricians and nurses, and they are being correctly diagnosed. There is, however, scope for improvement in aspects including comprehensive care planning and referral to epilepsy surgery services where children and young people meet relevant criteria.
Results by Health Board/Trust and regional network
Our detailed results spreadsheets (download these MS Excel files below) covers the Round 3 clinical audit data for cohort 1 and the 2019 organisational audit results.
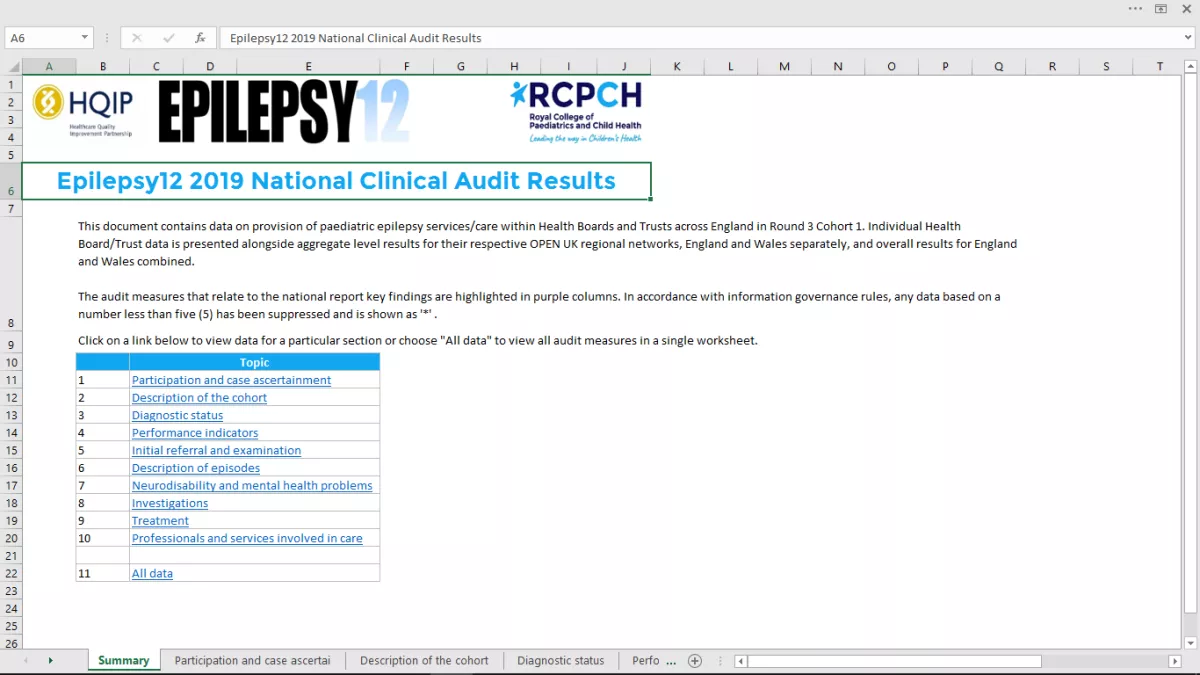
In the first tab, Summary, you can click on one of the 10 topics to see results for that topic, or 'All data' to see results for all topics. See below screenshot.
You can filter each worksheet to view and compare data for one or more NHS Health Boards/Trusts, or Regional Paediatric Epilepsy Networks, or you can view for all units in England and Wales.
The audit measures that relate to the national report's key findings are highlighted in purple columns.
- 1Joint Epilepsy Council of the UK and Ireland. (2011). Epilepsy prevalence, incidence, and other statistics
- 2Royal College of Paediatrics and Child Health (2020) State of Child Health in the UK. https://stateofchildhealth.rcpch.ac.uk/evidence/long-term-conditions/ep…